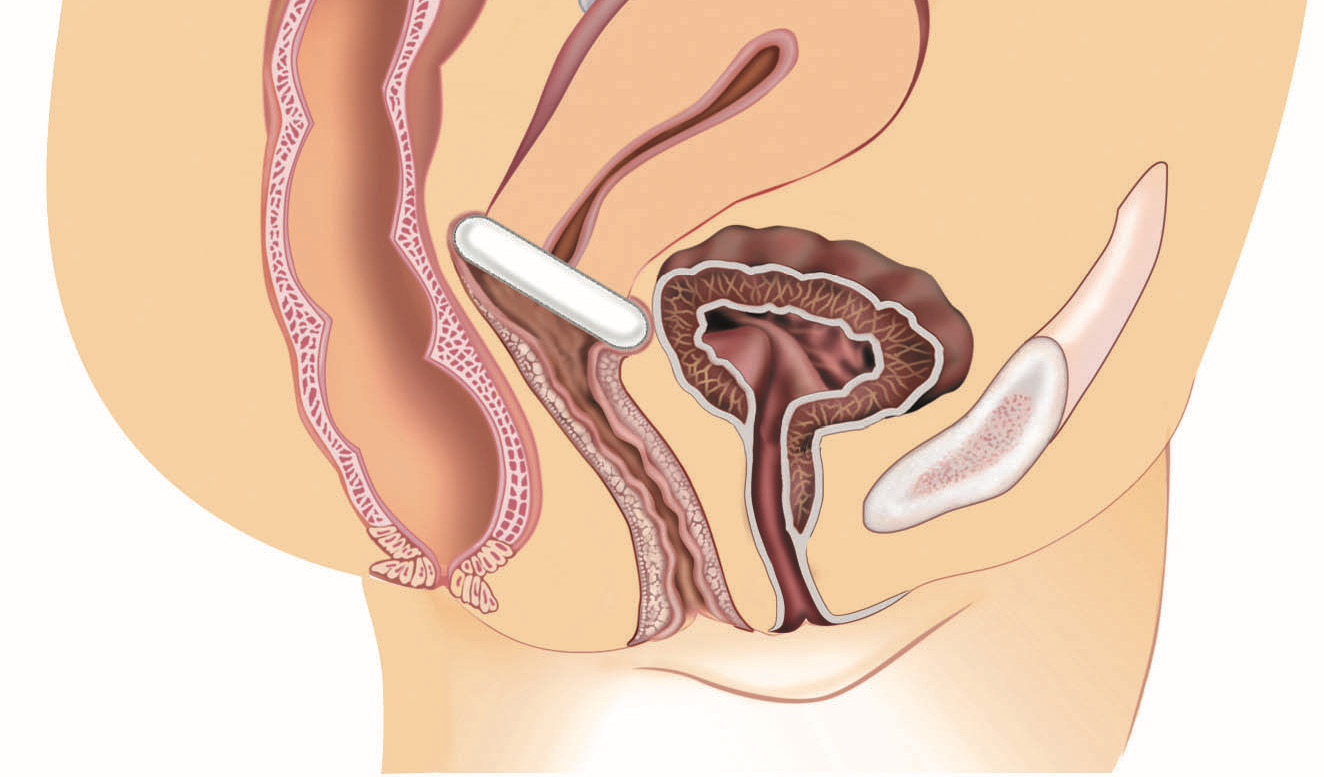
A pessary—a device inserted into the vagina to support pelvic organs in conditions like pelvic organ prolapse (POP) or stress urinary incontinence—is often presented as a simple, non-surgical solution. And for many women, it genuinely is. But like any medical device, understanding the downside of a pessary—including the risk of vaginal irritation, discharge, or the need for regular professional cleaning—is essential for making an informed choice about your pelvic health.
The main downsides of a pessary include vaginal discharge and odour, the need for regular removal and cleaning (or clinic visits), risk of vaginal erosion and ulceration, fitting difficulties, potential impact on sexual activity, and in some cases, worsening of urinary symptoms. Understanding these helps set realistic expectations.
The Most Common Pessary Problems
1. Vaginal Discharge and Odour
One of the most frequently reported complaints. A pessary is a foreign body in the vaginal environment – it disrupts normal flora and can cause:
- Increased vaginal discharge (often white-grey)
- Unpleasant odour – sometimes described as fishy (similar to bacterial vaginosis)
- This is not always infection – it can be a normal response to the device
Management: Regular pessary cleaning, vaginal oestrogen cream (improves vaginal health especially in post-menopausal women), and regular reviews.
2. Vaginal Erosion and Ulceration
If a pessary fits too tightly, is left in place too long without cleaning, or is used in a woman with atrophic vaginal tissue (common post-menopause), it can erode the vaginal wall – creating an ulcer or raw area.
| Risk Factor | Why It Increases Erosion Risk |
|---|---|
| Post-menopausal vaginal atrophy | Thin, fragile vaginal epithelium |
| Poor fitting | Pressure necrosis |
| Infrequent cleaning/removal | Tissue breakdown under chronic pressure |
| Certain pessary types | Rigid designs carry higher risk |
Erosion causes bleeding, pain, and discharge. It requires pessary removal and often local oestrogen therapy before resuming use.
3. Maintenance Requirements
Pessaries are not a set-and-forget device:
- Self-managed pessaries: must be removed, cleaned, and reinserted every 1-4 weeks
- Clinic-managed pessaries: require appointments every 3-6 months for removal, cleaning, and examination
- This ongoing commitment isn’t suitable for everyone – limited hand dexterity, poor eyesight, and anxiety about self-management are common barriers
4. Fitting Difficulties
Finding the right pessary size and type often requires several attempts:
- Approximately 20-30% of women cannot be successfully fitted
- Failed fitting reasons include: prolapse too severe, vaginal dimensions unsuitable, previous surgery altering anatomy
- Some women find fitting and removal uncomfortable despite optimal fitting
5. Impact on Sexual Activity
- Many pessaries (particularly ring pessaries without support) can remain in place during intercourse – but some women or their partners find this uncomfortable or psychologically off-putting
- Cube pessaries and some others must be removed before sex
- For women where sexual activity is important, this is a significant practical consideration
6. Worsening or Unmasking Urinary Symptoms
This is a counterintuitive but important issue:
- Some women with prolapse have masked stress incontinence – the prolapse has kinked the urethra and prevented leaking
- When a pessary corrects the prolapse, the kink is released and incontinence becomes apparent
- This is called occult stress incontinence and should be assessed before starting pessary use
Conversely, some pessaries (incontinence types) are designed to support the urethra and reduce stress leakage – but these aren’t appropriate for all prolapse types.
7. Rare but Serious Complications
| Complication | Signs | Action |
|---|---|---|
| Pessary migration / becoming embedded | Difficulty removing; pain | Urgent gynaecology review |
| Fistula formation (rare) | Urine or faeces from vagina | Emergency |
| Infection | Prompt medical attention |
Who Is NOT a Good Candidate
- Women unable or unwilling to manage the maintenance requirements
- Those with active vaginal infections (must treat before fitting)
- Women who had a prior pessary embedded or who had severe erosion
- Those who prefer a definitive surgical solution
The Bottom Line
Pessaries are a genuinely valuable tool for pelvic organ prolapse and incontinence – particularly for women who want to avoid or delay surgery, who are high surgical risk, or who are completing their families. But they are not without significant ongoing commitment and a meaningful side-effect profile. Discharge and odour, maintenance burden, fitting challenges, and risk of vaginal erosion are real limitations. A frank discussion with a urogynaecologist or women’s health physiotherapist about expectations, maintenance requirements, and personal preferences ensures the right decision is made.